- What are trigger points and how are they used in physical therapy?
- Signs and symptoms of trigger point pain
- What are the causes for a trigger point to start hurting?
- How to identify a myofascial pain point anywhere in the body?
- What is myofascial massage therapy and how can it help relieve trigger points?
- F.A.Q. Frequently Asked Questions
There are ailments that seem to have no apparent reason, appearing out of nowhere or after an injury that seemed to be 100% overcome. These pains are related to myofascial trigger points, which over time are created in the tissue that connects muscles with blood vessels, bones and nerves.
Knowing about this can improve your quality of life by solving this type of ailments that threaten to become chronic if not properly treated. Therefore, today you will learn in depth what trigger points are and the benefits of releasing them through physiotherapeutic massage.
What are trigger points and how are they used in physical therapy?
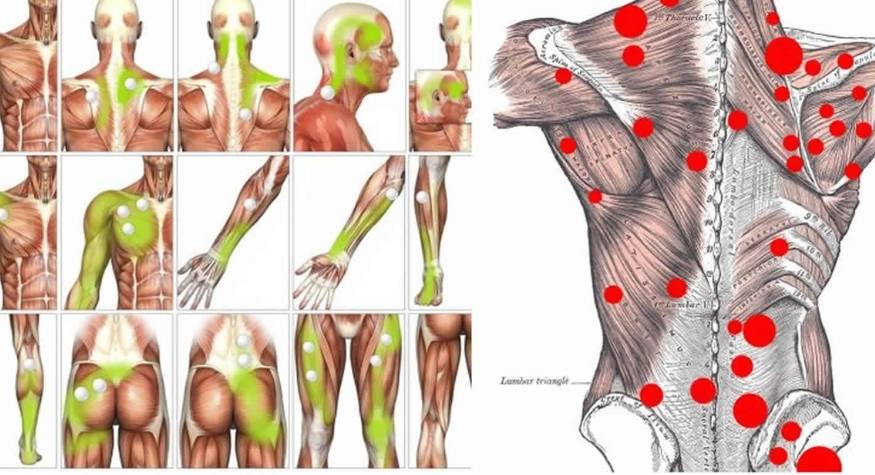
Myofascial pain points or trigger points are knots that are created in the deeper muscle tissues, causing intense pain. The pain does not always manifest itself right in the area where the point develops, but rather this pain is referred to nearby areas that seemingly do not appear to be related. In fact, it is estimated that more than 80% of the pain they cause manifests in other parts of the body.
In this sense you can imagine that a trigger point is similar to a herniated disc, which may appear in a specific vertebra of the spine, but the pain can manifest itself anywhere in the back as it is connected in its entirety by a large number of nerves. The same happens with the "trigger point" since the myofascial tissue is found throughout the body and is connected in its entirety.
Who and when was the existence of trigger points discovered?
The study of muscle pain dates back to the 15th century, but it was not until 1942 that Dr. Janet Travell coined the clinical term myofascial trigger point. Despite the impact of this doctor's work, not much further exploration was done until 1983, when Dr. Travell teamed up with Dr. David G. Simons and wrote the book " Myofascial Pain and Dysfunction - Trigger Point Manual".
This book would have 2 volumes that changed the way chronic pain worked in rheumatology and physiotherapy. In addition to providing a series of practical knowledge to treat various ailments without the need to resort to drugs.
What is fascia?
Fascia is a thin tissue that connects muscles with nerves, bones and blood vessels, which gives stability to the entire musculoskeletal system, and absorbs impacts from trauma, contusions or high-demanding sports. Although its main function is to be a connective tissue that allows all muscle complexes to work as one.
It is in the fascia where trigger points appear, as over the years it loses stability and contracts and shortens, causing the formation of these knots that proliferate to other muscle tissues and cause pain.
What is myofascial pain syndrome?
When the fascia accumulates myofascial pain points that are not released correctly, irreparable damage is created in which all this tissue is chronically shortened, which facilitates the appearance of more trigger points and generates constant pain throughout the musculoskeletal system.
Myofascial pain syndrome is diagnosed when a person suffers from many trigger points that appear repeatedly. It is at this point when myofascial release therapies should be performed constantly to relieve pain as much as possible without having to resort to the use of drugs and invasive surgical procedures.
bestseller
-
Acupressure Mat and Pillow (Green/Navy)
$49.95 -
Acupressure Pillow (Pink/Bordeaux)
$29.46 -
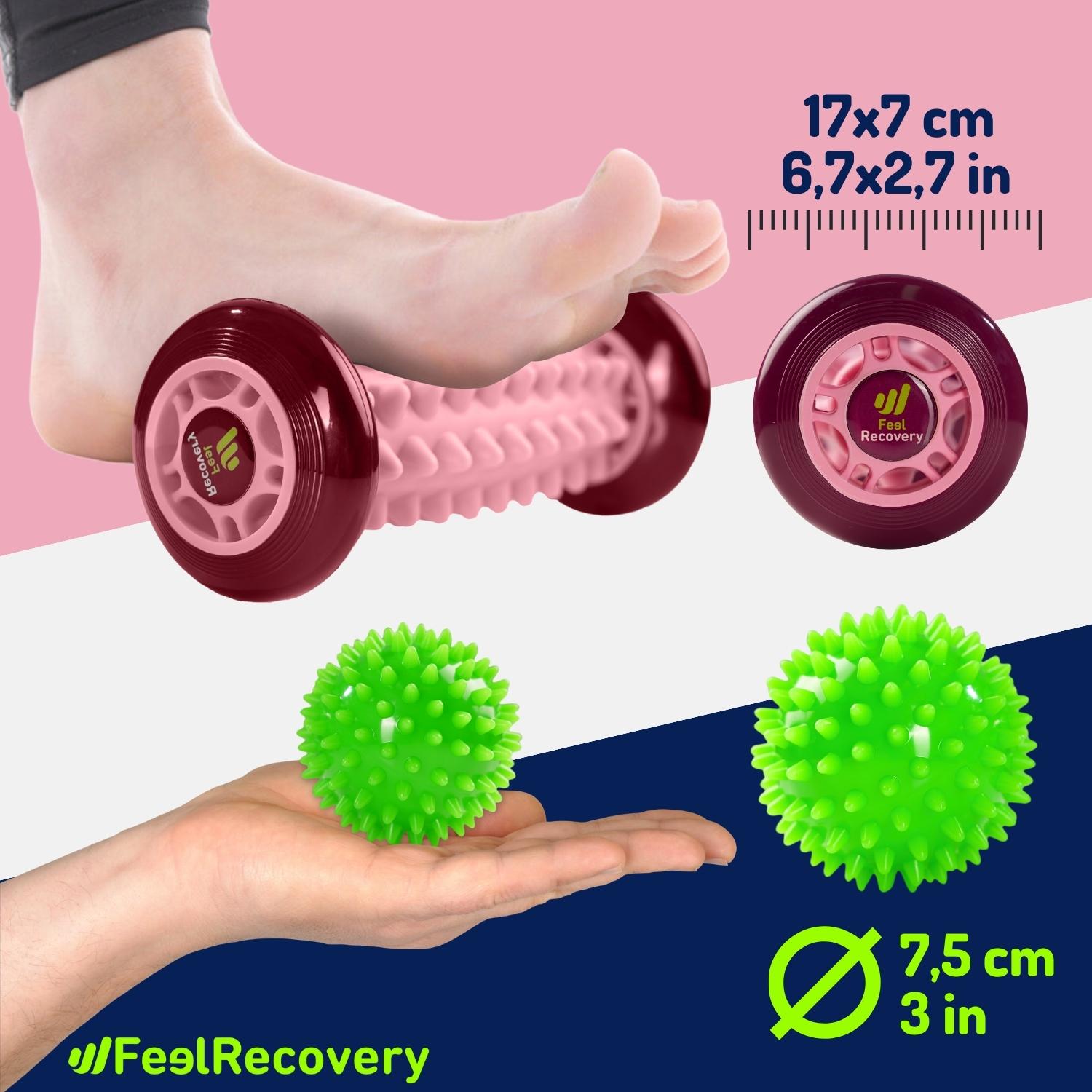
Foot Massage Roller for Plantar Fasciitis (Pink)
$19.95 -
High Density Foam Roller for Muscle (Black/Gray)
$29.95 -
High Density Foam Roller for Muscle (Pink/Bordeaux)
$29.95 -
Ice Massage Roller Ball (Green)
$39.95 -
Pack 2 In 1 Foam Roller High + Soft Density (Green/Navy)
$29.95 -
Soft Density Foam Roller for Recovery (Black)
$29.95 -
Trigger Point Massage Stick (Black)
$14.95
Signs and symptoms of trigger point pain
The pain caused by myofascial knots is very characteristic, but at the same time it can be confusing because it is very similar to the pain caused by a muscle contusion or contracture, or even a cramp. However, this pain has several characteristic symptoms that make it more recognizable.
Among them, the following stand out:
- The pain starts with low intensity until it intensifies.
- You will notice that the muscle where the trigger point is located is tight, to the point of feeling a knot to the touch.
- There may be pain in several parts of the body, indicating the existence of several trigger points.
- The pain is felt deep within the muscle, it is not as superficial as a contusion or muscle strain.
- It appears after prolonged sitting or standing.
- Weakness in the painful extremities.
- It disappears completely after a certain period of time.
What are the causes for a trigger point to start hurting?
A trigger point appears when the myofascial tissue suddenly shortens and contracts. This causes it to cut off its own blood supply, which irritates it further and causes the tissue around it to also begin to tighten, which can create pressure in nearby areas that are apparently unrelated to it.
So far, it is not known for certain why tissue shortening occurs in the first place, but among the most likely causes can be identified:
- Aging: over the years, muscles lose nutrients, elasticity and resistance, which makes these spasms in the myofascial tissue that generate the creation of trigger points more common.
- Poorly healed injuries: if the tissue of a muscle injury does not heal properly, it is likely that the damage is also reflected in the deep tissue, which will facilitate the creation of trigger points in the future.
- Poor nutrition and hydration: if muscles do not receive sufficient nutrients and hydration, especially during periods of intense training, they will be more susceptible to cramps, strains, contractures and of course myofascial knots.
There are other conditions and injuries that can cause trigger points to appear in muscles. Among the most common we can identify the following:
- Tendonitis.
- Herniated discs.
- Fibromyalgia.
- Carpal tunnel syndrome.
- Plantar fasciitis.
- TMJ dysfunction.
- Thoracic outlet syndrome.
- Post-polyomyelitis syndrome.
- Peripheral neuropathy.
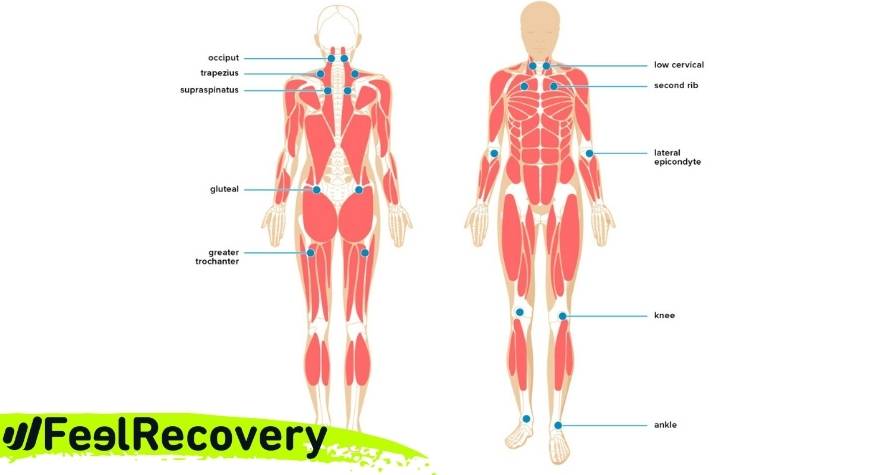
How to identify a myofascial pain point anywhere in the body?
Identifying where one of these points has appeared requires some expertise as it is not always reflected as a knot, but can sometimes also manifest as a rigid area that looks more like a "band" of muscle or a section of muscle that feels tight to the touch.
To locate a trigger point, each section of the painful area should be palpated in detail, but also its surroundings, since it is possible that it appears in a different area and the pain we feel is referred and not punctual. Sometimes it is necessary to apply a little pressure on the muscle in order to feel it, since it may originate in the deeper tissue.
In general, a friction with the fingertips in circular movements is usually performed. When locating the trigger point or band you will feel how this is more tense than the surrounding tissue, and possibly the patient will feel pain to the touch, although this will not always be the case.
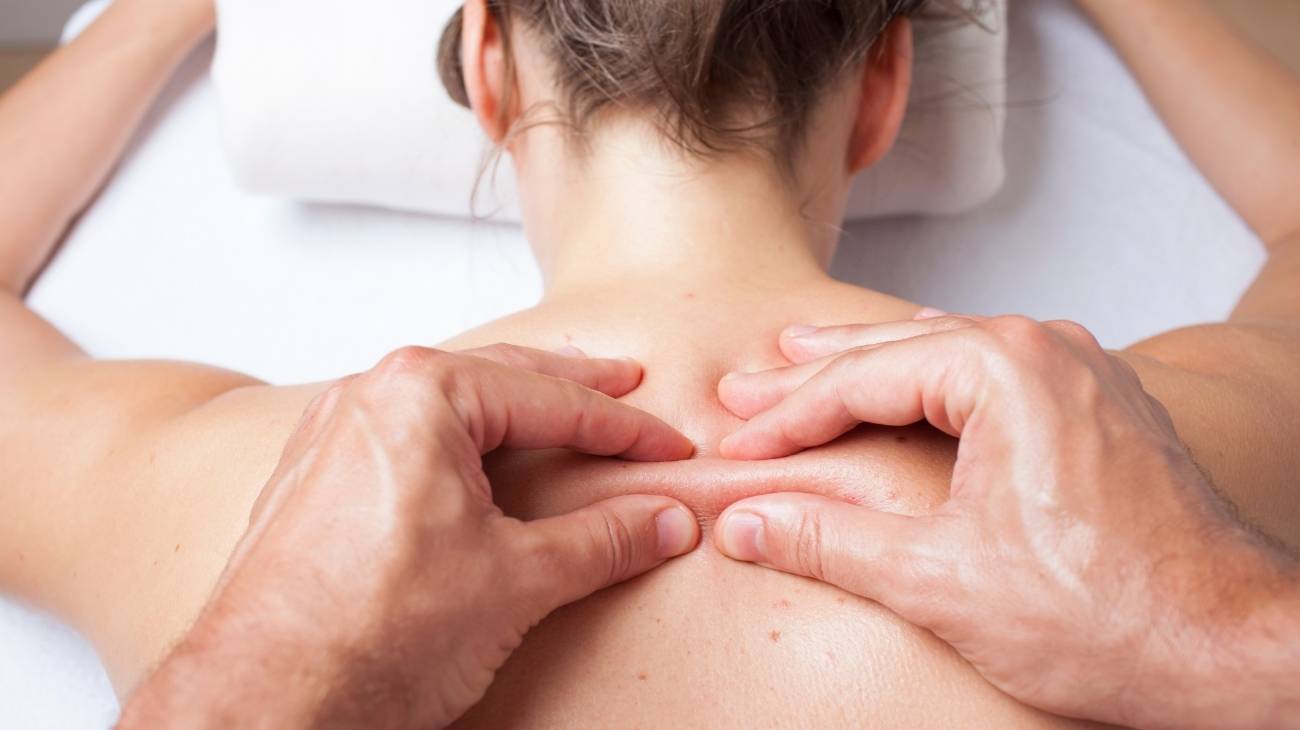
What is myofascial massage therapy and how can it help relieve trigger points?
Myofascial release therapy is a massage therapy focused on reducing and eliminating trigger points by releasing tension on the fascia so that the pain is relieved and does not recur. However, when the cause of the pain is due to myofascial pain syndrome, the relief from these sessions will only be temporary, because when it becomes a chronic problem the recurrence of pain will be constant.
What are the techniques of myofascial release therapy?
Myofascial release is based on the application of massage on trigger points to relieve muscle pain caused by the contraction and shortening of myofascial tissue. In essence, the same techniques of therapeutic massage are used, with the difference that the maximum effort is made on the aforementioned pain points.
Myofascial release techniques are divided into 2 types. Superficial release and deep release. Each of them is composed of a series of specific massage techniques to achieve a specific effect on the trigger point. Among the most prominent are:
- J-sliding: a technique in which the muscle tissue is slid and the hands "draw" a letter "J" with the movements made either with the palm of the hand or the fingertips.
- Friction: pressure is applied with the intention of generating a movement of the muscle tissue that causes the release and stretches the myofascial tissue concentrated in the trigger point.
- Vertical massage: with the fingertips or knuckles we proceed to perform a friction on the muscle fibers vertically so that the tissue is mobilized and release the pressure concentrated in the fascia.
What ailments can be treated with it?
In addition to myofascial pain syndrome, there are several ailments that generate pain that can be relieved by applying TLM to stimulate the relaxation of myofascial tissue.
Among them we can highlight:
- Tendonitis.
- Cervical pain.
- Back pain.
- Lumbalgias.
- Sciatica.
- Frozen shoulder.
- Fibromyalgia.
When should this therapy not be applied?
Although this therapy, being natural, does not carry any health risk, it is important to avoid it in case of suffering from any of the conditions mentioned below:
- Acute skin infections.
- Open wounds on the skin.
- Skin burns.
- Bone fractures.
- Severe arterial deficiency.
- Deep vein thrombosis.
F.A.Q. Frequently Asked Questions
References
- Simons, D. G., & Mense, S. (2003). Diagnosis and therapy of myofascial trigger points. Schmerz (Berlin, Germany), 17(6), 419-424. https://europepmc.org/article/med/14648314
- McPartland, J. M., & Simons, D. G. (2006). Myofascial trigger points: translating molecular theory into manual therapy. Journal of Manual & Manipulative Therapy, 14(4), 232-239. https://www.tandfonline.com/doi/abs/10.1179/106698106790819982
- Dommerholt, J., Bron, C., & Franssen, J. (2006). Myofascial trigger points: an evidence-informed review. Journal of Manual & Manipulative Therapy, 14(4), 203-221. https://www.tandfonline.com/doi/abs/10.1179/106698106790819991
- Lavelle, E. D., Lavelle, W., & Smith, H. S. (2007). Myofascial trigger points. Anesthesiology clinics, 25(4), 841-851. https://www.sciencedirect.com/science/article/abs/pii/S1932227507000687
- Alvarez, D. J., & Rockwell, P. G. (2002). Trigger points: diagnosis and management. American family physician, 65(4), 653. https://www.aafp.org/pubs/afp/issues/2002/0215/p653.html?userguid=unk-1632566170543&condition=other&clientId=&entityId=203
- Moldwin, R. M., & Fariello, J. Y. (2013). Myofascial trigger points of the pelvic floor: associations with urological pain syndromes and treatment strategies including injection therapy. Current urology reports, 14(5), 409-417. https://link.springer.com/article/10.1007/s11934-013-0360-7
- Vernon, H., & Schneider, M. (2009). Chiropractic management of myofascial trigger points and myofascial pain syndrome: a systematic review of the literature. Journal of manipulative and physiological therapeutics, 32(1), 14-24. https://www.sciencedirect.com/science/article/abs/pii/S0161475408002923
- Gonzalez-Perez, L. M., Infante-Cossio, P., Granados-Nunez, M., Urresti-Lopez, F. J., Lopez-Martos, R., & Ruiz-Canela-Mendez, P. (2015). Deep dry needling of trigger points located in the lateral pterygoid muscle: efficacy and safety of treatment for management of myofascial pain and temporomandibular dysfunction. Medicina oral, patologia oral y cirugia bucal, 20(3), e326. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4464920/
- Shah, J. P., Thaker, N., Heimur, J., Aredo, J. V., Sikdar, S., & Gerber, L. (2015). Myofascial trigger points then and now: a historical and scientific perspective. PM&R, 7(7), 746-761. https://www.sciencedirect.com/science/article/abs/pii/S1934148215000799
- Lucas, N., Macaskill, P., Irwig, L., Moran, R., & Bogduk, N. (2009). Reliability of physical examination for diagnosis of myofascial trigger points: a systematic review of the literature. The Clinical journal of pain, 25(1), 80-89. https://journals.lww.com/clinicalpain/Abstract/2009/01000/Reliability_of_Physical_Examination_for_Diagnosis.12.aspx