- What is Achilles tendon bursitis?
- What are the causes and risk factors for bursitis of the heel of the foot?
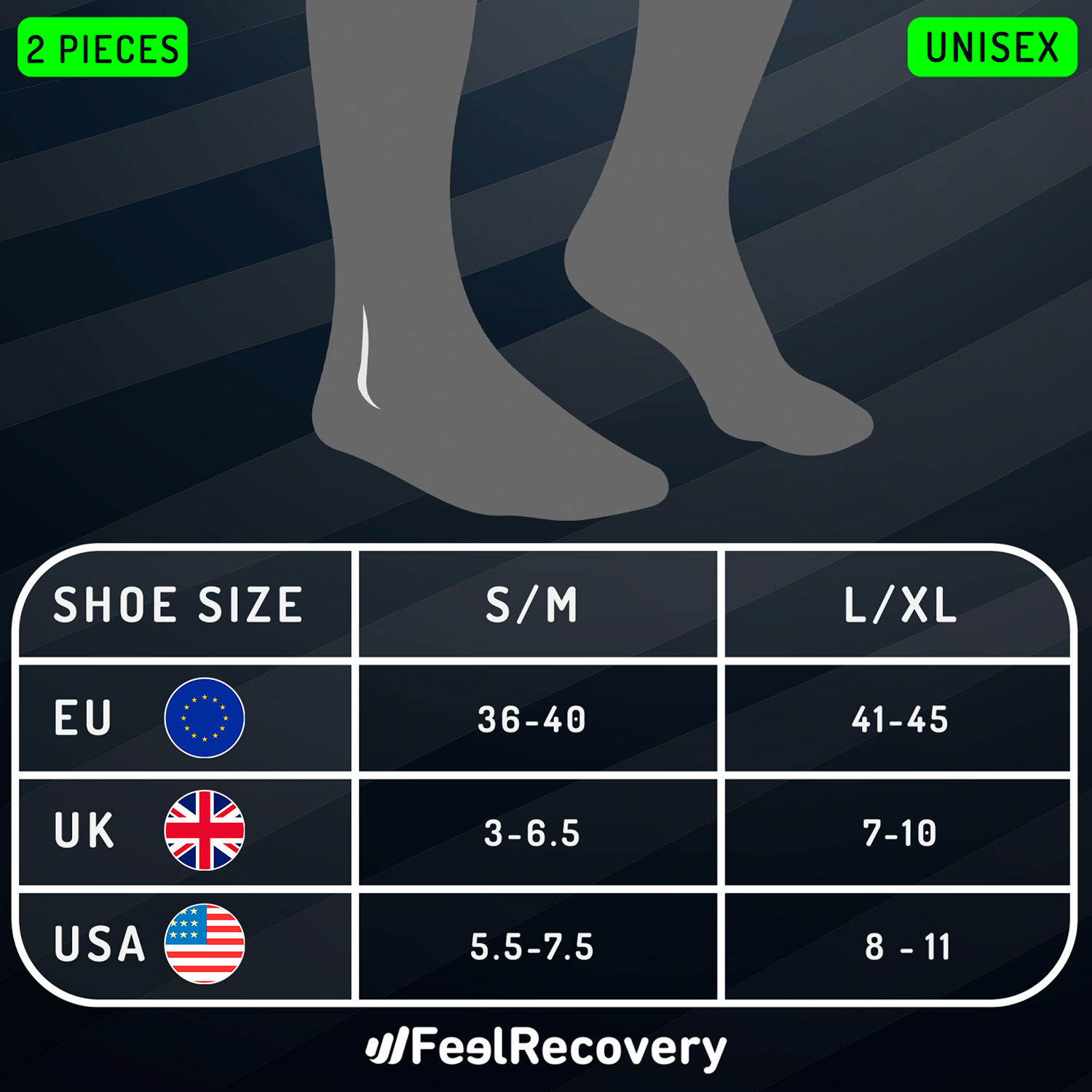
- Best products for Achilles bursitis
- Main symptoms that warn us that we have Achilles bursitis
- What treatments are available to improve the symptoms of Achilles tendon bursitis?
- What are the most effective prevention methods for heel bursitis?
In Achilles tendon bursitis, it is necessary to see a doctor as soon as possible to prevent the inflammation in the retrocalcaneal and subcutaneous calcaneal bursae from progressing and, therefore, gradually increasing the excess synovial fluid in them. For this reason, it is a good idea to know what this disease is and what causes it.
We invite you to continue reading because in the following paragraphs you will find all the information related to this ailment generated in the ankle. You will also learn about the symptoms and treatments that will help you to reduce the inflammation. Let's get started.
What is Achilles tendon bursitis?
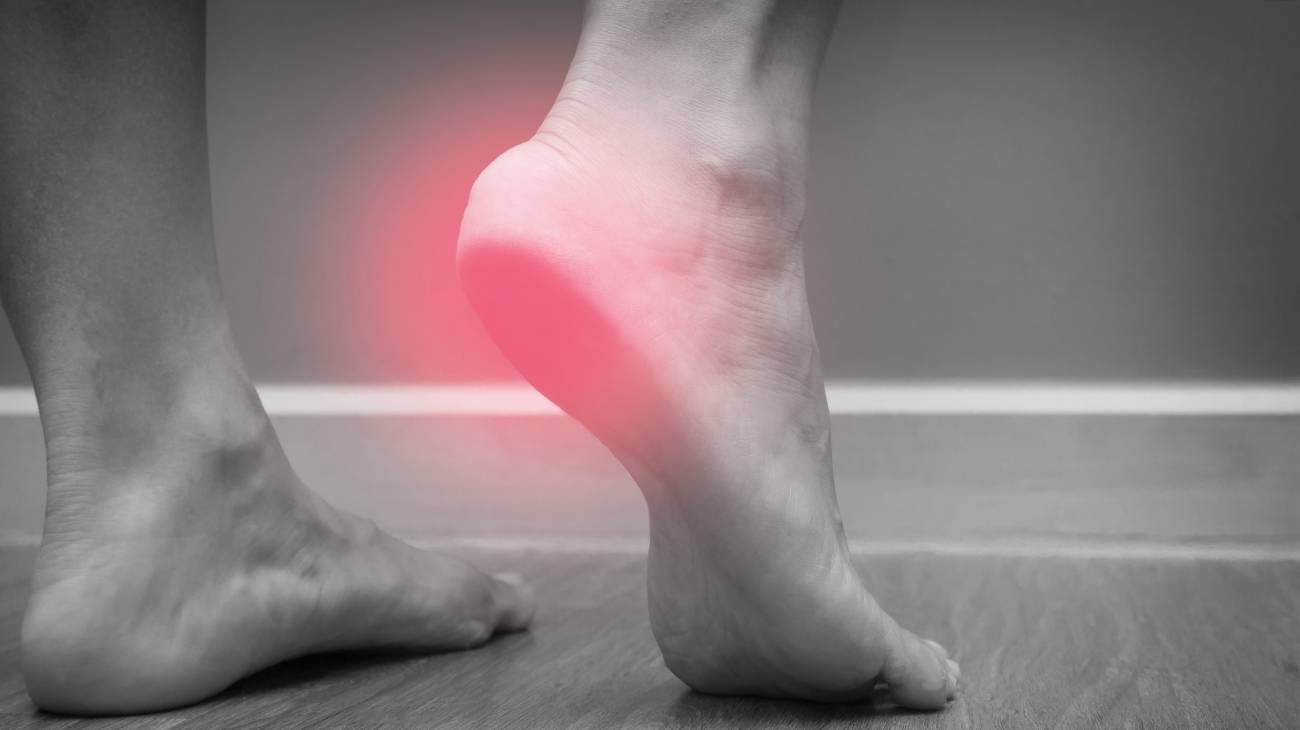
Achilles tendon bursitis is an inflammatory, non-degenerative and painful condition that occurs in the heels of the foot. It occurs when any of the retrocalcaneal or subcutaneous calcaneal bursae are exposed to pressure, infection or other pathological factors for a prolonged period of time. It should be borne in mind that these flattened bursae contain synovial fluid in order to minimise the friction caused by movement at the heel.
The abnormality present in these sacs located between the calcaneal bone and the Achilles tendon (tissue in charge of connecting the soleus, plantaris delta and gastrocnemius muscles with the bony formation) causes swelling, loss of mobility and redness in the area. Bursitis can be treated with conventional therapies and, in more severe cases, with surgery.
What are the causes and risk factors for bursitis of the heel of the foot?
Older people are more prone to suffer from subcutaneous calcaneal bursitis, due to the deformation that occurs in the bones. But it is important to clarify that this is not the only risk factor that can lead to the inflammatory disease.
Here is a list of other recurring causes of Achilles bursitis
- Tight-fitting shoes: shoes with high heels exert a continuous impact on the ankle joint when moving. This constant pressure irritates the bursae, causing a build-up of synovial fluid, which leads to bursitis.
- High-impact activities: activities such as walking, jumping, running or jogging are normal. However, if overdone, the bursa will be exposed to more stimulation than it can handle, causing lubrication to be needed to keep the bones from touching. This increases synovial fluid.
- Trauma: receiving blows to the top of the heel can cause an inflammatory abnormality in the serous bursa. Not only do they swell, but oedema sometimes occurs due to blood retention from bruising.
- Overloading: when the heel joint area is subjected to long-term movements with excessive weight, either on the body or by lifting heavy items, the joint is subjected to more pressure than normal and the bursae may swell.
- Inflammatory rheumatoid arthritis: This disease damages the joints in the tissues, so the synovial bursae are not exempt from damage. In fact, arthritis is potentially most damaging to the small areas of the limbs. There are different reasons for this, but the most common is the poor bone formation that arthritis causes, resulting in less opening of the synovial sacs.
- Gout disease: Gout with its deposits of uric acid in the body of the joints also plays a role in the inflammation of the synovial sacs. When these crystalline concentrations occur, the tissues and bursae swell and cause pain.
- Bone disorders: various abnormalities in the bones of the foot usually create extra pressure in the synovial sacs. This is due to the narrow cavity connecting tendon, bone and bursa. For example, high plantar arches in Haglund's syndrome is linked to Achilles tendon bursitis.
- Infectious bacteria: for various reasons, whether injuries or breaks in the skin, harmful bacteria can lodge in the synovial capsules, one of the most common pathogens being gram-positive cocci. Upon infection, the body reacts with various immune system defence mechanisms by increasing the level of fluid in the heel.
- Poor diet: patients who include high-fat foods in their diets can lead to the accumulation of microcrystals in the hyaline cartilage. This creates bone spurs, which we discussed in previous sections.
- Sedentary lifestyle: lack of exercise causes the muscles and tendons to lose their elasticity and firmness. This causes the slightest sudden or abrupt movement to stress the area, causing injuries that can lead to an increase in synovial fluid in the bursae of the heel.
Best products for Achilles bursitis
Bestseller
-
2 Ankle Compression Sleeve (Black/Gray)
$19.95 -
2 Ankle Compression Sleeve (Green/Navy)
$19.95 -
2 Ankle Compression Sleeve (Pink/Bordeaux)
$19.95 -
Ice Pack for Foot - Cold Therapy Socks (Black)
$24.95 -
Ice Pack for Foot - Cold Therapy Socks (Green)
$24.95 -
Ice Pack for Foot - Cold Therapy Socks (Pink)
$24.95 -
Microwavable Heated Slippers (Hearts)
$24.95 -
Microwavable Heated Slippers (Oxford)
$24.95 -
Microwavable Heated Slippers (Sport)
$24.95 -
Microwaveable Heating Pad for Pain Relief (Hearts)
$19.95 -
Microwaveable Heating Pad for Pain Relief (Oxford)
$19.95 -
Microwaveable Heating Pad for Pain Relief (Sport)
$19.95 -
Sport Compression Socks (1 Pair) (Black/Gray)
$19.95 -
Sport Compression Socks (1 Pair) (Green/Navy)
$19.95 -
Sport Compression Socks (1 Pair) (Pink/Bordeaux)
$19.95
Main symptoms that warn us that we have Achilles bursitis

For this reason, it is useful to know the most characteristic signs of this disease:
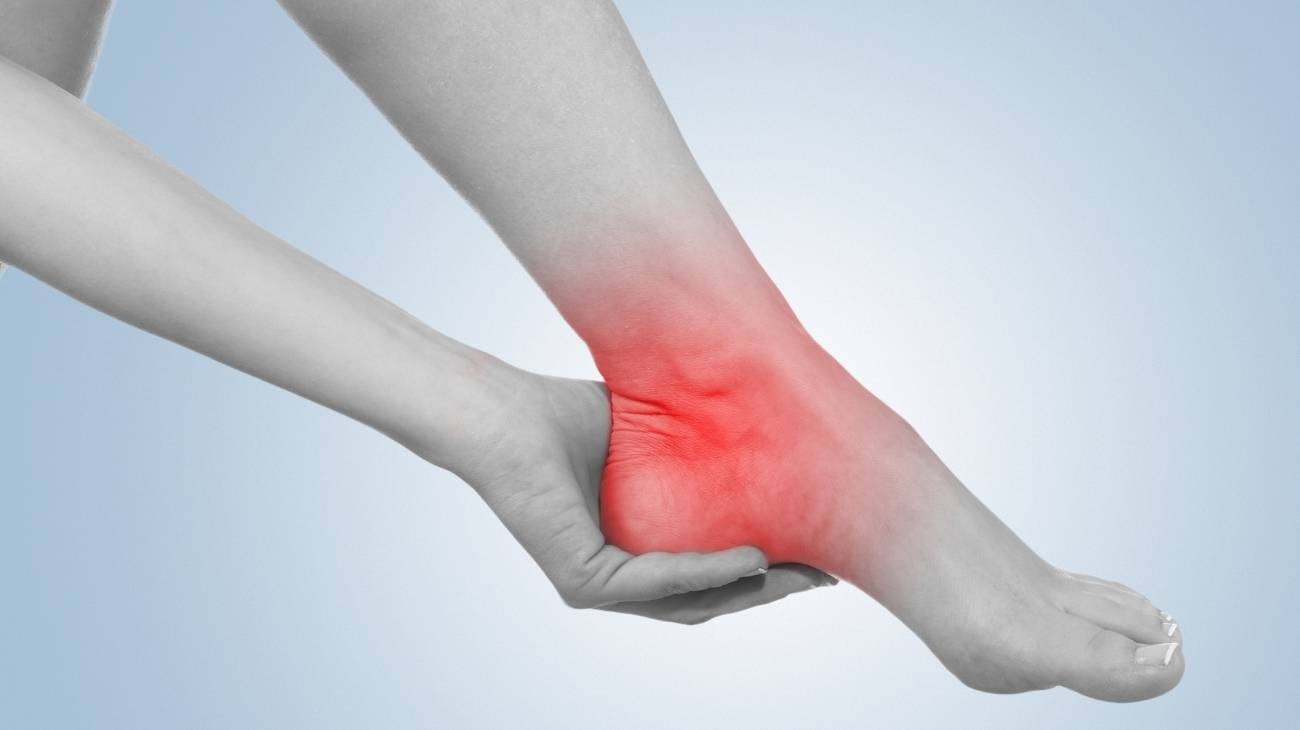
- Shooting pain: Bursitis is not a normal or favourable situation for the patient. Therefore, the body alerts in advance by triggering a nerve response that is perceived as intense, sharp pain in the heel.
- Tingling sensation: if overload, trauma or other factors attack the joint, they not only damage the tissues and bones, but also the nerves present in the region. As a result, tingling and numbness may occur.
- Loss of sensation: like the symptom of paraesthesia mentioned in the previous point, temporary loss of sensation in the heel is a common sign of chronic bursitis. This is associated with nerve damage triggered by prolonged swelling and other related pathologies.
- Increased pain when performing movements: because the soft tissue of the bursa is irritated, any movement not only causes pain, but also aggravates it. This is especially true for actions that involve raising, lowering or rotating the foot. An easy way to find this out is to climb a ladder or stand on your toes. If more pain appears, it is advisable to see a doctor as a matter of urgency.
- Reddening of the skin: the increased blood supply to the affected area causes redness. This is why the patient may notice a very reddish hue on the back of the foot.
- Feeling of warmth: sometimes the patient feels a higher temperature at the heel, just at the back of the foot. This symptom is a consequence of a higher blood flow to the affected area.
- Fever: unlike a passing hot sensation, fever is an abnormally high temperature in the region. If such a sign increases, it is possible that septic bursitis is latent and needs prompt medical attention.
- Skin erosion: although the disease is internal, the body tends to produce noticeable external changes. That is, in addition to being red and tender, the affected area may have an abnormal texture.
What treatments are available to improve the symptoms of Achilles tendon bursitis?
When the patient is diagnosed, treatment focuses on improving the condition of the synovial bursa of the heel. Above all, this area is rested, deflated and healed as quickly as possible, perhaps by immobilising the whole foot or the back of the foot. In addition, other therapies and joint treatments may be recommended, which we will discuss below.
Alternative and complementary therapies
The aim of these types of treatment is to reduce the symptoms and cause the disease to go into remission. We will show you below the most commonly used therapies:
- Hot and cold therapy: alternating cold compresses on the heel with heat-emitting elements reduces inflammation and pain by activating blood flow and muscle and tendon relaxation. The hot or cold gel packs should be rested on the problem area for a few minutes to prevent burns. About 15 to 20 minutes is more than enough.
- Compression therapy: The use of compression ankle braces is common in cases of Achilles tendon bursitis. This goes hand in hand with immobilisation, compression and resting the foot on soft areas such as pads. While these ankle pads compress the tendon, they relieve the pressure in the area generating an effective compressive effect.
- Massage therapy: to carry out this treatment, be careful and ask the doctor if it is feasible to apply it to the Achilles heel. He/she will most likely say that it can only be performed by a professional, who will avoid stressing the joint and will not put pressure on the bursae.
- Acupressure therapy: as with massage therapy, it is possible to use this oriental technique based on pressure on different parts of the body only with the therapist's hands. But this must be applied by an acupressure practitioner.
- Thermotherapy: the application of heat to the heel is one of the most commonly used techniques to alleviate the symptoms of this inflammatory disease. It can be applied by means of electric blankets, water bags or cold gels to the affected area. This will stimulate the dilatation of the blood vessels, thus reducing inflammation in the region and relaxing the muscle-tendon structure.
- Natural remedies using plants: footbaths are baths that can be applied to the feet to cause relaxation and a feeling of well-being in the extremities. Generally, mint, ginger, rosemary, willow and citrus fruits are used. It is also possible to ingest infusions that provoke relaxation, such as boldo, lime blossom and camomile.
- Healthy lifestyle habits: to avoid future injuries and improve the symptoms of bursitis, it is necessary to re-educate the patient. This consists of getting them to make changes in their daily life. For example, it is recommended to exercise, not to smoke or drink alcohol, to eat healthy, to adopt correct posture, etc.
Nutritional supplements
Treatment with supplements of magnesium, manganese, selenium and even chondroitin sulphate and glucosamine, the latter two present in hyaline cartilage, can be applied to reduce inflammation and improve the functioning of the synovial bursae located in the Achilles heel. Keep in mind that this therapy is recommended only by the doctor, so the dosage and frequency of intake must be prescribed to avoid future complications.
Physical therapy treatments
Physical therapy consists of the patient being subjected to different techniques that help to improve the opening of the joint and reduce inflammation in the bursae.
The most common techniques used by physiotherapists include:
- Exercises: repetitions, stretching and heel movements are established; these include plantar flexion, eversion, inversion and dorsiflexion. In addition, it is possible to find multiple workouts focused on improving coordination and balance.
- Low-level laser therapy: In cases where conservative treatment has been ineffective, low-frequency laser therapy can be effective. In this technique, infrared light is applied with a device to the injured area to energise the cells and encourage repair. Best of all, it is a painless therapy with few side effects.
- Microcurrents: Microcurrent therapy is widely used for retrocalcaneal disorders. A low-intensity electrical signal is emitted, imperceptible to the human eye, which activates the electrochemistry of the soft tissues.
- Contrast baths: the difference with hot and cold therapy is that in this treatment, exercises are performed under water at different temperatures. It consists of immersing the feet in cold water and then in hot water, but not too hot. This alternates the hot and cold baths multiple times until relief, reduction of swelling and cessation of pain is achieved. It should be applied under the supervision of a health specialist, who moves the joint with gentle and constant movements.
Medications
The first thing to clarify is that pharmacological therapy must be applied by a doctor, who will determine the extent of the illness and the types of medication to be prescribed. Therefore, self-medication is never beneficial.
It can cause internal bleeding, liver and gastrointestinal disorders, beyond aggravating the symptoms of Achilles bursitis. Anti-inflammatory drugs, corticosteroids and, in more severe cases, injectable antibiotics are among the drugs of choice for Achilles bursitis.
Surgery and fluid removal
This type of treatment is only used in severe cases. Drainage of the synovial fluid can be applied by means of a small valve placed in the affected area or by needles where the excess fluid is deposited in syringes. Alternatively, if the above treatment was unsuccessful, the patient is likely to be referred for surgery to remove the affected bursae, this is known as a bursectomy.
What are the most effective prevention methods for heel bursitis?
The heavy mechanical work of the ankle and heel makes this area prone to inflammation of the bursae. It is therefore advisable to take care of the Achilles heel and prevent bursitis so that the joint is always in good working order.
We will show you below different preventive methods that you should take into account
- Perform warm-up exercises: it is advisable, before any physical activity, to perform warm-up exercises so that the neuromuscular and cardiorespiratory systems begin to activate. This will increase the viscosity of the synovial fluid in the bursae.
- Wear appropriate and comfortable footwear: Since the heels bear the entire weight of the body, and has constant movement and friction, it is essential to wear comfortable footwear. This will help cushion the impact of walking, running and climbing more gently. In this way the bursae will work simply with the correct joint width, avoiding excess synovial fluid.
- Use orthopaedic insoles: these are designed to maintain a uniform footprint. It is useful for everyone, but especially for athletes, workers and those with a tendency to plantar abnormalities. This avoids malformations such as the appearance of osteophytes that end up causing retrocalcaneal bursitis.
- Do not make sudden movements: if mild inflammation or overload is suspected, it is not wise to continue making movements that cause pain. Stop pushing the bursa to the limit is one of the primary preventive measures to avoid injury.
- Eat healthy and avoid a sedentary lifestyle: always choose a balanced diet rich in vitamin D and Omega 3 will help you maintain a healthy joint, which will keep the bursae in your feet from becoming inflamed. This will also be enhanced by walking or cycling for at least 30 minutes a day if you spend a lot of time sitting.
References
- Van Dijk, C. N., Van Sterkenburg, M. N., Wiegerinck, J. I., Karlsson, J., & Maffulli, N. (2011). Terminology for Achilles tendon related disorders. Knee Surgery, Sports Traumatology, Arthroscopy, 19, 835-841. https://link.springer.com/article/10.1007/s00167-010-1374-z
- Mazzone, M. F., & McCue, T. (2002). Common conditions of the Achilles tendon. American family physician, 65(9), 1805-1811. https://www.aafp.org/pubs/afp/issues/2002/0501/p1805.html
- Schepsis, A. A., Jones, H., & Haas, A. L. (2002). Achilles tendon disorders in athletes. The American journal of sports medicine, 30(2), 287-305. https://journals.sagepub.com/doi/abs/10.1177/03635465020300022501
- Mathieson, J. R., Connell, D. G., Cooperberg, P. L., & Lloyd-Smith, D. R. (1988). Sonography of the Achilles tendon and adjacent bursae. American Journal of Roentgenology, 151(1), 127-131. https://www.ajronline.org/doi/abs/10.2214/ajr.151.1.127
- Kleinman, M., & Gross, A. E. (1983). Achilles tendon rupture following steroid injection. Report of three cases. JBJS, 65(9), 1345-1347. https://journals.lww.com/jbjsjournal/Citation/1983/65090/Achilles_tendon_rupture_following_steroid.19.aspx
- McAfee, J. H., & Smith, D. L. (1988). Olecranon and prepatellar bursitis. Diagnosis and treatment. Western Journal of Medicine, 149(5), 607. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1026560/
- Reilly, D., & Kamineni, S. (2016). Olecranon bursitis. Journal of shoulder and elbow surgery, 25(1), 158-167. https://www.sciencedirect.com/science/article/abs/pii/S1058274615004693
- Khodaee, M. (2017). Common superficial bursitis. American family physician, 95(4), 224-231. https://www.aafp.org/pubs/afp/issues/2017/0215/p224.html
- Rasmussen, K. J. E., & Fanø, N. (1985). Trochanteric bursitis: treatment by corticosteroid injection. Scandinavian journal of rheumatology, 14(4), 417-420. https://www.tandfonline.com/doi/abs/10.3109/03009748509102047
- Sayegh, E. T., & Strauch, R. J. (2014). Treatment of olecranon bursitis: a systematic review. Archives of orthopaedic and trauma surgery, 134, 1517-1536. https://link.springer.com/article/10.1007/s00402-014-2088-3