Tendonitis, commonly known as tendinopathy, is a condition characterized by inflammation or irritation of a tendon. Tendons are the fibrous tissues that connect muscles to bones, facilitating movement. When subjected to repetitive strain or overuse, they can become inflamed, causing symptoms like pain, swelling, and reduced flexibility. Effective treatment and recovery strategies are crucial for restoring function and preventing chronic conditions.
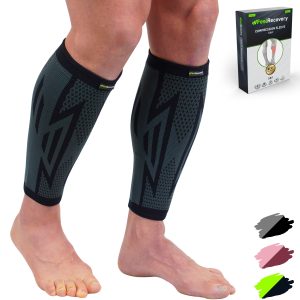
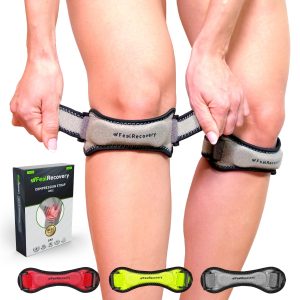
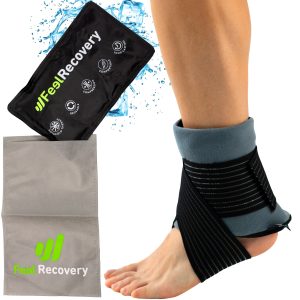
One of the most effective treatments for tendonitis is compression therapy. Compression sleeves are designed to apply targeted pressure to the affected area, reducing swelling and improving blood flow. This enhanced circulation delivers essential nutrients and oxygen to the damaged tendons, speeding up the healing process.
Cold therapy is highly beneficial in the early stages of tendonitis. Ice packs or cold wraps reduce inflammation and numb the affected area, providing quick pain relief. Using cold therapy immediately after an activity that exacerbates the pain can prevent further damage and inflammation.
Heat therapy becomes useful as the condition progresses. Heat wraps or pads relax tense muscles and improve flexibility by increasing blood flow. This approach is especially helpful before rehabilitation exercises to prepare the tendons and surrounding muscles for activity.
Electrotherapy devices, such as TENS units, are an excellent option for managing tendonitis-related pain. These devices deliver low-frequency electrical impulses that block pain signals and promote the release of endorphins. Incorporating electrotherapy into your recovery plan can enhance overall comfort and support long-term healing.
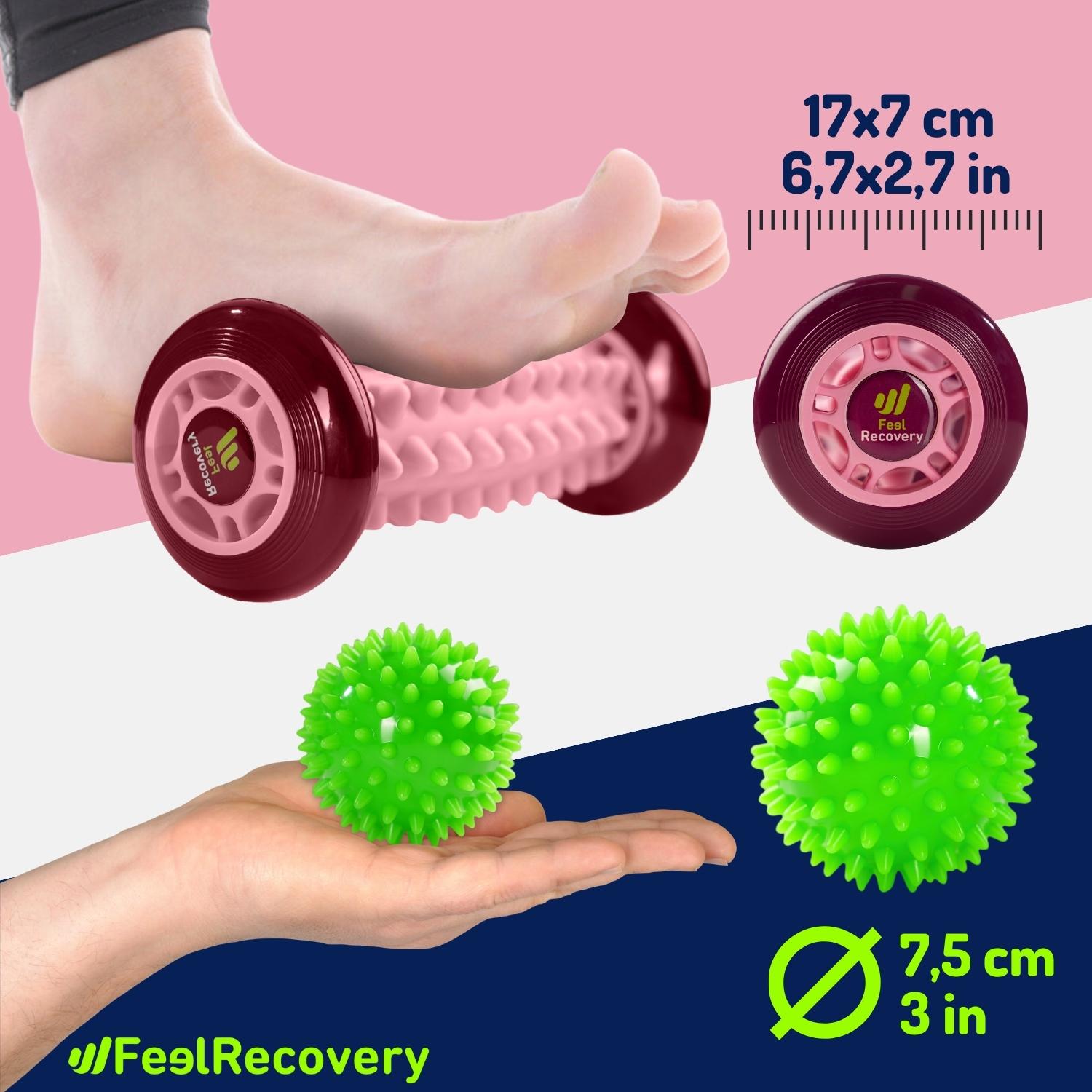
Massage therapy is another effective method for addressing tendonitis. Using massage tools or professional techniques can help reduce stiffness, improve blood circulation, and relax the affected tendons. Massage, combined with heat therapy, offers a comprehensive approach to alleviating discomfort and promoting recovery.
Strengthening exercises play a pivotal role in tendonitis recovery. Resistance bands are highly effective for controlled, low-impact exercises that rebuild strength and stability in the affected tendons. Regular use of resistance bands can reduce the risk of reinjury and improve overall tendon health.
Investing in high-quality recovery tools tailored to tendonitis can significantly improve your healing process. From compression sleeves and cold therapy wraps to electrotherapy devices and massage tools, these products offer targeted relief and comprehensive care. By integrating these solutions into your daily routine, you can restore functionality, reduce pain, and prevent future flare-ups effectively.
FAQ: Frequently Asked Questions
What is the most effective treatment for tendonitis?
The most effective treatments for tendonitis include a combination of compression therapy, cold and heat treatments, and targeted rehabilitation exercises to reduce pain and inflammation while promoting healing.
When should I use heat versus cold therapy for tendonitis?
Cold therapy is ideal during the initial stages to reduce inflammation and pain, while heat therapy is more beneficial later to improve flexibility and prepare for rehabilitation exercises.
Are TENS units effective for tendonitis pain?
Yes, TENS units help manage tendonitis pain by delivering electrical impulses that block pain signals and stimulate endorphin release, providing significant relief.
How do resistance bands help with tendonitis recovery?
Resistance bands provide controlled, low-impact exercises that strengthen the affected tendons and surrounding muscles, reducing the risk of reinjury and improving overall stability.
Can massage therapy improve tendonitis recovery?
Yes, massage therapy helps by reducing stiffness, improving blood circulation, and relaxing the affected tendons, making it an effective complementary treatment for tendonitis.